Arteriovenous Malformation Embolization:
Arteriovenous malformations (AVMs) are congenital tangles of blood vessels that can occur inside the brain. AVM's may be diagnosed after bleeding in the brain, after a seizure or may be discovered incidentally on a scan. Because AVMs pose a risk of bleeding, it is sometimes recommened that they be treated with embolization, explained below. Embolization is generally performed prior to neurosurgical removal of an AVM and aides the neurosurgeon in the safe removal of the abnormal brain tissue.
Most patients with an AVM undergo a diagnostic angiogram of the brain in advance of treatment to best assess the extent of the abnormality. After a plan is made by the treating physicians, a patient is scheduled to return to the neurointerventional suite and placed under general anesthesia. While asleep, embolization occurs. During this process, the arteries of the body are accessed through an artery of the leg. A microcatheter is placed inside the blood vessels of the AVM. Through the microcatheter, the arteries of the AVM are injected with the glue-like substance (n-BCA or Onyx) to block blood flow to the AVM.
Large AVMs may require more than one treatment procedure, scheduled over several weeks. After embolization is complete, most patients have the abnormal brain tissue neurosurgically removed.
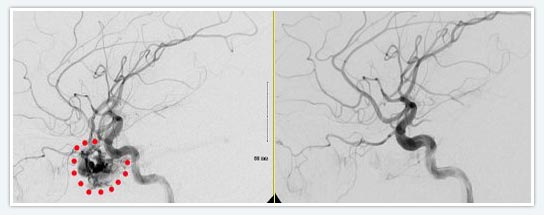
Arteriovenous malformation (circled in red) before and after embolization with n-BCA
by the neurointerventional team at Saint Luke's Hospital of Kansas City.
Dural AV Fistulas
Dural arteriovenous fistulas (DAVFs) are closely related to AVMs. Rather than congenital, DAVFs develop in life's later years. They may cause bleeding in the brain and, under many circumstances, treatment with glue embolization is recommended. Often DAVFs can be cured with glue embolization alone and neurosurgery is not required.
| 








